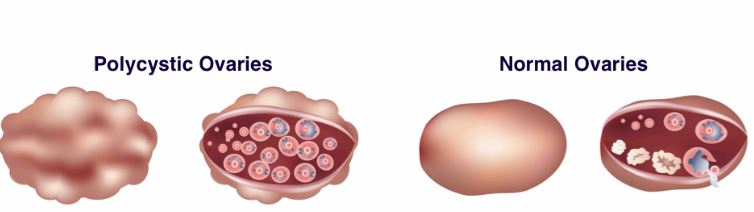
Polycystic ovary syndrome (PCOS) is currently the most common hormone abnormality among the reproductive-aged women. It occurs in as much as 10% of the women that are in this reproductive group. Polycystic ovary syndrome is characterized by menstrual abnormalities, overproduction of androgen testosterone, and the presence of enlarged ovaries, which contain multiple polycystic ovaries (small follicles).
A woman who has severe PCOS will have an excess of androgen, resistance to insulin, abdominal fat, menstrual irregularities, and will be at a greater risk of getting cardiovascular and diabetes diseases, as compared to a woman who has a less severe form of polycystic ovary syndrome.
Here’s an infographic that summarizes what you need to know about PCOS.

The condition is more common amongst family members as compared to randomness. This suggests that family genes play a major role in PCOS development. The severity of this condition can also be affected by a person’s lifestyle preferences e.g. exercise and dieting. Weight gain can, therefore, worsen both metabolic and reproductive abnormalities.
As a result, polycystic ovary syndrome can adversely impair your health by increasing your risks of:
- Infertility
- Cardiovascular disease
- Obstetrical complications
- Diabetes
What is PCOS?
Polycystic ovary syndrome also referred to as Stein-Leventhal syndrome has been categorized as one of the most prevalent hormonal endocrine maladies in a woman. The condition has been diagnosed and recognized for more than seventy-five years. You are likely to experience a number of signs and symptoms if you have this condition.
Given that it is not possible to diagnose it using a single test, and the fact that the symptoms experienced by different women are likely to vary, it has come to be referred to as “The Silent Killer.” Prompt diagnosis of this condition is vital, as it has been linked to increased risks of developing various medical conditions, including insulin resistance and heart blood pressure.
According to Mayo Clinic, 40% of women who have been diagnosed with glucose intolerance and diabetes between the ages of twenty and fifty have this syndrome. Additionally, there are studies that have established that if a mother has the syndrome, there exists a 50% probability that the daughters will also suffer from the same condition.
However, the good news is that proper education and prompt diagnosis can assist in lowering your risk factors, allowing you to live a happy and healthy life.
What are the main causes of Polycystic Ovary Syndrome?
To-date, the exact cause of this syndrome is yet to be known, though many doctors have a belief that genetics and hormonal imbalances play an active role in its development. Additionally, a woman has a higher chance of developing the condition if her sister or mother has this syndrome.
Another contributing factor for its development is the excess production of the androgen hormone. Even though androgen is a male hormone, it is also produced by the women’s bodies. Therefore, if you have PCOS, it means that your body is producing very high amounts of androgen above normal rates, which in return upsets the creation and release of your eggs when ovulating. High androgen levels in your body can be caused by the production of excess amounts of insulin.
PCOS Symptoms
Traditionally, the symptoms start to appear as soon as you have started menstruating, and even though they could be mild in the beginning, they may worsen with time. Additionally, you should note that the type and severity of the signs and symptoms will vary from one woman to the next. Apart from experiencing an irregular menstrual flow, additional symptoms may include:

- Trouble losing weight and weight gain
- Acne
- Thinning hair on your scalp
- The emergence of extra hair on your face and body.
- Depression
- Fertility problems
- Decrease in overall breast size
- Pelvic pain
- Development of a deeper voice
Even though they are not symptoms of this condition, most women who have polycystic ovary syndrome will also have concurrent health diseases e.g. high cholesterol, diabetes, and hypertension. All three conditions are linked to the increase in weight, which is typical for women with this syndrome.
Diagnosis
For a PCOS verdict to be made by your physician, they have to review your symptoms, perform various tests, and review your medical history in a bid to rule out the possibility of other conditions. A pelvic and physical examination has to be performed so as to look for the syndrome’s symptoms such as swollen clitoris or swollen ovaries.
Additionally, blood tests to quantify the woman’s sex hormones are naturally ordered, along with:
- Fasting glucose tests—these are for measuring blood sugar levels
- Thyroid function tests—they are used to determine the amount of thyroid hormones being produced by your body
- Lipid tests— are for determining the amount of cholesterol that is present in the blood stream
- Vaginal ultrasound—it allows the gynecologist to develop real-time images of the woman’s reproductive organs
- Pelvic Laparoscopy—a surgical technique where the doctor inserts a tiny camera to determine whether there are growths in your ovaries after making a small incision in the abdomen.
What are the risk factors?
With PCOS, the main risk factor is an existing family history. Your chances of getting this condition improve significantly if there are women in your family who have had it or who happen to have diabetes or irregular menstrual periods. This condition can be passed from either your father’s or mother’s side.
Note:
- Having a family history of PCOS condition increases your chances of getting PCOS because the strong relationship that exists between the syndrome and diabetes.
- Long-term usage of seizure related medicine e.g. Depakote has also been linked to increased risks of getting the condition.
Treatment
It is impossible to prevent or cure polycystic ovary syndrome, but, it is possible to manage its symptoms. You can manage the symptoms using the options discussed below:
1. Lifestyle changes
For obese women, the overall risk of getting long-term health complications associated with the syndrome may be enhanced significantly by taking measures to shed the excess weight. Losing as much as 5% of your extra weight has the potential to lead to significant improvements in the syndrome.
It is probable to establish whether you are of healthy weight by calculating your BMI (body mass index). It is a measurement of your current weight levels in relation to your existing height. A normal body mass index should be between 18.5 to 24.9.
The extra weight can be shed by taking up regular exercises, as well as ensuring that your diet is healthy and well-balanced. The diet should include both fruits and vegetables and should be at least five portions in a single day. It should also comprise of whole foods e.g. brown rice and wholegrain cereals, as well as chicken, lean meats, and fish.
2. Medications
You can use a variety of medications to address some of the symptoms you experience as a result of having this condition. They include:
Absent or irregular periods
The contraceptive pill comes highly recommended in inducing regular periods. You can also use an intermittent course of progesterone pills. Using these pills also reduces your long-term risks of getting endometrial cancer (cancer of the womb lining), which is common among women who do not get regular periods.
Fertility problems
With the right treatment, a woman who has this condition can become pregnant. Normally, a woman is started on a short course of pills, which she has to take when starting her cycle, and one’s that are to be taken for a number of cycles.
If the pills are not successful, the physician may recommend IVF treatment or injections. But, you should note that with this kind of treatments, there is always an increased risk of getting multiple pregnancies.
Unwanted hair loss and growth
Some of the medications that are issued to control alopecia (hair loss) and hirsutism (excess hair growth) include:
- Certain types of combined oral pills e.g. Yasmin
- Finasteride
- Flutamide
The medications function by blocking performance of the “male hormones,” while others suppress their production by your ovaries.
Surgery
LOD (laparoscopic ovarian drilling) is a minor surgery, which can also be used in treating fertility-related problems, which could be associated with this syndrome. The doctor first administers general anesthesia before making a small cut in the lower part of the tummy.
A thin microscope will then be passed through the minor incision into the tummy. Your ovaries will then be treated using laser or heat in order to get rid of the tissue that is behind the production of the androgen hormones. The surgical procedure has been seen to lower LH and testosterone hormone levels while increasing the levels of the FSH. By so doing, it corrects the existing hormonal imbalance, which may then lead to the restoration of the normal functioning of your ovaries.
PCOS and Pregnancy
When you have procystic ovary syndrome, you are at a higher risk of getting pregnancy-related complications e.g.
- High blood pressure
- Miscarriage
- Gestational diabetes
- Pre-eclampsia
In case you happen to be overweight, you can always lower your risks of getting such complications by exercising and dieting to eliminate the extra weight before you attempt to get a baby.
Home Remedies for PCOS
Even though a viable treatment has yet to be found for this particular problem, it is still possible to get it under control. Apart from some of the medications that have been mentioned above, you can use the following home remedies to get the symptoms under control, as well as reduce the PCOS related complications.
1. Cinnamon
Columbia University researchers have been able to establish that cinnamon supplementation in your everyday diet can assist in improving your menstrual cyclicity. Also, a study recently published in the Journal of Fertility and Sterility has indicated that cinnamon herb can also be used to reduce insulin resistance among women suffering from this problem.
What to do at home
- Add a single teaspoon of cinnamon to a cup of warm water. Take the solution each day for the next few months
- Alternatively, consult your doctor about taking this herb in the form of a supplement. Typically, it is recommended that you take a single capsule each day.
Note: you should not intake more than two tablespoons of cinnamon powder in one day. For women taking it to combat their insulin resistant, they need first to consult their doctors, as the herb can lower their blood sugar levels.
2. Flaxseed
Flaxseed can also be used in combating the symptoms associated with this syndrome, as it assists in decreasing the androgen levels in the body. In addition, it happens to be very high in fiber, and this makes it possible for it to lower cholesterol levels, as well as slow down the glucose metabolism rates.
It contains omega-3 fatty acids, which lower blood pressure as well as reduce bodily inflammation.
What to do at home
- Combine two tablespoons of freshly ground seeds in a single cup of water. You will be required to take this solution each day for the next few months
- Additionally, you can consider including the ground seeds in your everyday diet by adding it to your salads, smoothies, or soups.
3 fenugreek
It has been known to promote the metabolism of glucose in your body as well as in improving insulin resistance. In turn, it assists in balancing body hormones. In addition, it can aid in weight loss and in lowering your cholesterol.
What to do at home
- Take three tablespoons of these seeds and soak them in a bowl of warm water for six hours. On an empty stomach, take a single spoonful of the soaked seeds with honey. Take the seeds in the morning, and ten minutes before taking your lunch or dinner.
- Alternatively, include the seeds in your regular diet
If you think that you have this condition, you should speak with your GP immediately so that the necessary tests can be run. Early PCOS diagnosis makes it possible for you to manage its symptoms, allowing you to continue living your normal life.
Article resources
- NHS Choices Staff. (N.D): http://www.nhs.uk/conditions/periods-absent/Pages/Introduction.aspx
- Mayo Clinic Staff. (2014, September 3). Polycystic ovary syndrome: http://www.mayoclinic.com/health/polycystic-ovary-syndrome/DS00423/DSECTION=treatments-and-drugs
- Polycystic ovary syndrome. (N.D.): http://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0024506/
- Moran, L. J., Norman, R. J., & Teede, H. J. (2015, March). The metabolic risk in PCOS: Phenotype and adiposity impact [Abstract]. Trends in Endocrinology & Metabolism, 26(3), 136–143.
http://www.cell.com/trends/endocrinology-metabolism/abstract/S1043-2760(14)00206-9 - Polycystic ovary syndrome (PCOS) fact sheet. (2016, January 5): https://www.womenshealth.gov/publications/our-publications/fact-sheet/polycystic-ovary-syndrome.html